The Company is developing dronabinol for the treatment of OSA, a sleep-related breathing disorder that afflicts an estimated 29 million people in the United States and an additional 26 million in Germany and 8 million in the United Kingdom. OSA involves a decrease or complete halt in airflow despite an ongoing effort to breathe during sleep. When the muscles relax during sleep, soft tissue in the back of the throat collapses and obstructs the upper airway. OSA remains significantly under- recognized, as only 20% of cases in the United States and 20% of cases globally have been properly diagnosed. About 24 percent of adult men and 9 percent of adult women are believed to have the breathing symptoms of OSA with or without daytime sleepiness. OSA significantly impacts the lives of sufferers who do not get enough sleep; their quality of sleep is deteriorated such that daily function is compromised and limited. OSA is associated with decreased quality of life, significant functional impairment, and increased risk of road traffic accidents, especially in professions like road and rail transportation and shipping.
Research has established links between OSA and several important co-morbidities, including hypertension, type II diabetes, obesity, stroke, congestive heart failure, coronary artery disease, cardiac arrhythmias, and even early mortality. The consequences of undiagnosed and untreated OSA are medically serious and economically costly. According to the American Association of Sleep Medicine, the estimated economic burden of OSA in the United States is approximately $162 billion annually. All current treatment options have serious drawbacks. We believe that a new drug therapy that is effective in reducing the medical and economic burden of OSA would have major benefits for the treatment of this costly disease indication.
Continuous Positive Airway Pressure (“CPAP”) is the most common treatment for OSA. The cpap supplies work by blowing pressurized air into the nose (or mouth and nose), which keeps the pharyngeal airway open. Patients must use the device whenever they sleep.
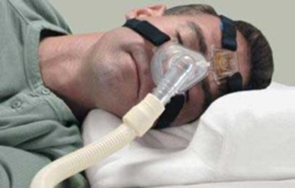
Reduction of the apnea-hypopnea index (“AHI”) is the standard objective measure of therapeutic response in OSA. Apnea is the cessation of breathing for 10 seconds or more and hypopnea is a reduction in breathing. AHI is the sum of apnea and hypopnea events per hour. In the sleep laboratory, CPAP is highly effective at reducing AHI. However, the device is cumbersome and difficult for many patients to tolerate. Most studies describe that 25-50% of patients refuse to initiate or completely discontinue CPAP use within the first several months and that most patients who continue to use the device do so only intermittently. To avoid that, experts tend to recommend people to use a supplementary humidifier with the device or use distilled water (you can buy distilled water uk or wherever you are based if interested) in the CPAP device that can help reduce the uneasiness while using it.
Oral devices may be an option for patients who cannot tolerate CPAP. If you’re having trouble sleeping, your sleep doctor may also recommend trying different types of mattresses until you find one that suits you. Several dental devices are available. The cost of these devices tends to be high and side effects associated with them include night-time pain, dry lips, tooth discomfort, and excessive salivation. Patients with clinically significant OSA who cannot be treated adequately with CPAP or oral devices may elect to undergo surgery, the most common form of which involves the removal of excess tissue in the throat to make the airway wider. Patients who undergo surgery for the treatment of OSA risk complications. Surgery is often unsuccessful, and at present, no method exists to reliably predict therapeutic outcome from surgery.
In 2014 another surgical option became available based on upper airway stimulation. It is a combination of an implantable nerve stimulator and an external remote controlled by the patient. The implanted device stimulates the hypoglossal nerve, which controls the tongue. The device is turned on at night and off in the morning by the patient with the remote.
